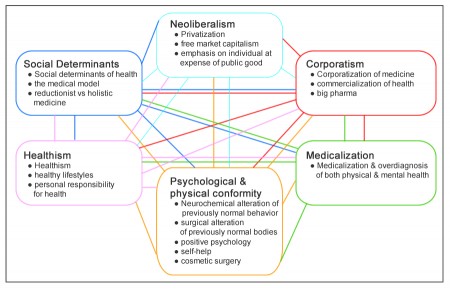
Continued from part one, where I discussed the first three of my six interests: healthism, medicalization, and psychological and physical conformity. Click on the graphic below to see a larger image.
The social determinants of health
Social determinants of health (often abbreviated SDOH) refers to unequally distributed social and economic conditions that correlate with unequal and inequitable distributions of health and disease. Presumably there is a causal relationship between the two, not merely a correlation. Definitively identifying the causal mechanisms, however, is difficult. A great many things influence our health (including things we’re not even aware of yet), and it can be difficult to isolate and scientifically study some of the ones we strongly suspect, like poverty, isolation, or a sense of being socially inferior.
The medical model is the preferred framework in modern westernized societies for explaining the distribution of health and disease. It emphasizes risk behavior (smoking, diet), clinical risk factors (blood pressure, blood sugar, cholesterol levels), genetics, health care access and quality, behavioral change, and patient education. One common characteristic of the medical model’s explanation of health and disease is that causes are located in the individual (behavior, genes), not in the individual’s economic and social environment.
In psychiatry, the medical model refers to the assumption that ‘abnormal’ behavior is the result of a physical problem (physiological, biochemical, and/or genetic) and should be treated with a medical intervention such as pharmaceutical drugs.
Reductionist vs. holistic medicine refers to the way the medical profession considers and treats patients. Modern scientific medicine is reductionist in that it understands disease by analyzing increasingly more minute biological entities (cells, molecular interactions, DNA). Reductionist medicine confines its interests not only to isolated individuals, but to isolated parts of the body (as in medical specialties).
Holistic medicine considers individuals in their environments. It was common until the late 19th century, and there was an unsuccessful attempt to revive holism in the 1930s. Much of the appeal of alternative health practices today is their holistic approach to the individual.
In a society that places a high value and financial priority on the medical model and reductionist medicine, it is difficult to implement policies that acknowledge the social determinants of health.
Neoliberalism
Neoliberalism refers to a set of economic assumptions: government policies should favor the wealthy since wealth will “trickle down” (supply-side economics); markets work best when there is no interference from government (free trade, deregulation); public services (education, health care, utilities) operate most efficiently (and profitably) when run as private businesses. Neoliberalism gives priority to the ideology of the individual at the expense of social welfare policies (e.g., Thatcher’s famous “There is no such thing as society”).
Neoliberalism is associated with the economic theory of Milton Friedman and the political policies of Margaret Thatcher and Ronald Reagan. The shift to neoliberal policies that began in the 1970s and 1980s has had a significant impact on health, social welfare, and the medical profession. The recent battle by health care professionals in the UK against government mandated privatization of the National Health Service (NHS) was an attempt to resist the application of neoliberal policies to health care (see Jonathan Jonathon Tomlinson on A better NHS).
The corporatization of medicine
I think of this topic as having three stages that blend into each other. The commodification of health encourages the public to view health goods and services as just another commodity (the patient as consumer). The commercialization of health is the recognition by business interests of just how profitable the health field can be. The corporatization of medicine is simply a more advanced stage of commercialization, where businesses compete with each other, consolidate into corporate entities, and concentrate on profits in order to maximize returns to shareholders.
The fallacy in this whole arrangement – a fallacy that makes commercialized and corporatized medicine highly detrimental to the physical, mental, and financial well being of the public — is that health is profoundly different from commodities that are typically bought and sold in a market economy (see From MD to MBA: The business of primary care). For more on the disastrous consequences of corporatized medicine in the US, see Maggie Mahar’s excellent book Money-Driven Medicine. For a discussion of the situation in the UK, see Tomlinson on Patients not Profits. How Markets dehumanise health.
I single out the pharmaceutical industry for inclusion in this category for several reasons: its corporate nature (shareholder profits take precedence over the health and safety of consumers); its direct sales appeal to consumers (DTC advertising in the US); and its enormous influence on the very nature of the science of medicine (on this see Corporate Science and the Husbandry of Scientific and Medical Knowledge by the Pharmaceutical Industry (PDF)).
Continued in part three, where I enumerate the (now obvious, I presume) connections that unite what I once saw as a collection of unrelated parts.
Related posts:
Why medicine is not a science and health care is not health
The physical exam and society’s regard for physicians: A history
The politics behind personal responsibility for health
Complaints about pharma go way back … to ancient Rome
Patient safety and corporate profits
From MD to MBA: The business of primary care
Are the most heavily marketed drugs the least beneficial?
References:
Jonathan Jonathon Tomlinson, A better NHS, Abetternhs’s Blog, July 19, 2011
Sara Henderson and Alan Petersen (editors), Consuming Health: The Commodification of Health Care (2001)
Maggie Mahar, Money-Driven Medicine: The Real Reason Health Care Costs So Much (2006)
Jonathan Jonathon Tomlinson, Patients not Profits. How Markets dehumanise health., Abetternhs’s Blog
Alastair Matheson, Corporate Science and the Husbandry of Scientific and Medical Knowledge by the Pharmaceutical Industry (PDF), Biosocieties (2008), 3, pp 355–382


Sorry, comments are closed for this post.