 This may seem like a ‘Debbie downer‘ subject to bring up right before a holiday, but I’d like to say a few words about death. Death is the elephant in the room whenever we talk about health, medicine, or healthcare. When we ‘eat right’ and exercise, we engage in a modern ritual that we hope will prevent something that’s 100 percent certain. Even the transhumanists, who hope to prolong life indefinitely, admit that eventually everyone will succumb to an übervirus or accidentally cross the path of a flying car.
This may seem like a ‘Debbie downer‘ subject to bring up right before a holiday, but I’d like to say a few words about death. Death is the elephant in the room whenever we talk about health, medicine, or healthcare. When we ‘eat right’ and exercise, we engage in a modern ritual that we hope will prevent something that’s 100 percent certain. Even the transhumanists, who hope to prolong life indefinitely, admit that eventually everyone will succumb to an übervirus or accidentally cross the path of a flying car.
The high tech flash of post-industrial medicine encourages this illusion, and that creates interesting problems. How do you allow someone to die a dignified and peaceful death when the focus of medicine is to keep everyone alive, even the terminally ill? What does it mean to die when modern medicine can keep us technically ‘alive’? Claus von Bulow’s wife Sunny has been in a coma for 28 years. It may seem crass to think about economics when we’re talking about a human life, but a high tech death in an ICU has implications for the high cost of healthcare.
The natural death: Genug Syndrome or Zahl Kam Rauf
It’s now rare to die of ‘natural’ causes in one’s own home. There are small pockets of resistance, however. A recent essay in JAMA called “Genug Syndrome” told the story of an elderly woman named Lisa. She had been cared for at home for eight years and died peacefully, sitting in her candy-apple-red wheelchair, surrounded by family and friends. When it came time to fill out the death certificate, the family decided she had died of genug syndrome. Genug is Yiddish for “Enough!” or “Enough, already!” When someone inquired about the actual cause of death, Lisa’s daughter objected. She didn’t want her mother’s life summed up by a medical diagnosis. The doctor agreed:
Should I mar the identity of this complex person with such a rich life and legacy by reducing her to a medical diagnosis at the end – when, really, it was just genug? When end-of-life care transcends the medical model to be truly a natural part of life, as this family had achieved, listing a medical-model cause of death seemed incongruent with her whole life and spirit.
The bureaucracy is stacked against doctors who resist filling out death certificates with a ‘medical-model’ cause of death. Fortunately this particular doctor (Jennifer Soyke) practiced in Oregon, a state that legalized euthanasia in 1994. She mentions a recent Oregon obituary that lists the cause of death as “the common form of Zahl Kam Rauf.” ‘Zahl kam rauf’ literally means ‘number came up.’
The certificate of death
Death certificates are designed to provide epidemiological information. The statistic-collectors want to know the leading causes of death by age, race, and sex. Instructions for death certificates are quite firm. You should never list the cause of death as cardiac or respiratory arrest. We already know that someone who is dead is not breathing. You must list the etiology, that is, the causal sequence of events that explains the final outcome: Type I diabetes mellitus resulting in renal failure, coronary artery arteriosclerosis resulting in cardiac arrest.
The CDC (Centers for Disease Control & Prevention) instructions (PDF) for filling out a death certificate specifically exclude a natural cause of death.
The elderly decedent should have a clear and distinct etiological sequence for cause of death, if possible. Terms such as senescence, infirmity, old age, and advanced age have little value for public health or medical research. Age is recorded elsewhere on the certificate.
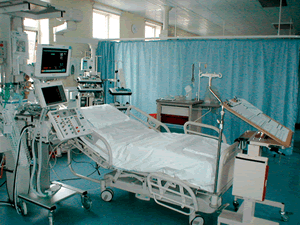 Here we confront the stark reality of modern medicine: It extends our lifespan (thank you very much) while it prolongs the dying process. Not only do drugs and surgical interventions buy us time. News bulletins from the research front keep us primed for breakthroughs that might buy us time if not a complete cure. Perhaps we won’t have to die after all. Surely part of the agony of being HIV+ must be the hopes that are so frequently extended and withdrawn.
Here we confront the stark reality of modern medicine: It extends our lifespan (thank you very much) while it prolongs the dying process. Not only do drugs and surgical interventions buy us time. News bulletins from the research front keep us primed for breakthroughs that might buy us time if not a complete cure. Perhaps we won’t have to die after all. Surely part of the agony of being HIV+ must be the hopes that are so frequently extended and withdrawn.
Death be not visible
Eighty percent of us will die in a hospital or long-term care facility. About twenty-five percent of hospitalized patients are in ICUs or cardiac care units before they die. Everything about an ICU conspires to keep the patient alive, as Sharon Kaufman describes:
Clinical medicine in the ICU is like surgery–its gaze falls only on a carefully circumscribed field, the analyzable interior of the body. A waning life is rendered invisible, or nearly so, in the reading and then treating of signs of the body’s pathology. Disease is treated until there is no more physiologic response to therapy. Only then is death expected. Only then does it “need” to be acknowledged by hospital staff.
This is modern, post-industrial death, where dying is a failure of the patient, the doctor, and medicine itself.
 It wasn’t always like this. Only recently has life expectancy reached three-quarters of a century in developed nations. Before the sanitary conditions of asepsis were discovered in the late 19th century, hospitals were charitable institutions for the poor, and anyone who could avoid them would do so.
It wasn’t always like this. Only recently has life expectancy reached three-quarters of a century in developed nations. Before the sanitary conditions of asepsis were discovered in the late 19th century, hospitals were charitable institutions for the poor, and anyone who could avoid them would do so.
When life was shorter, death loomed larger. It was nearer. It was more familiar, and familial — people usually died at home, surrounded by family, and an extended, non-nuclear family at that. Neighbors and passersby would see the black-creped door and come by to pay their respects. This was how the dying made their passage, and were passed on by the living, to whatever comes next.
Today, death is a more clinical affair. We die in hospitals. We mourn in private. We cremate the dead. We might see a line of cars, linked by their headlights into an orderly procession, and know they’re headed for the cemetery. But such motorcades are not as common as they used to be. And aside from emergency rooms, hospital waiting rooms, and accident scenes, death has gradually disappeared from public view.
The peaceful death
Daniel Callahan, a distinguished bioethicist who writes on health policy, would like to reclaim the premodern, more visible death; a death “that is accepted without overpowering fear and a death that has lost its power to terrorize.” He advocates a ‘peaceful’ death, one that combines the social and emotional advantages of a premodern death with the palliative resources available from modern medicine. Biomedicine keeps us alive longer, but it can also reduce suffering and improve the quality of life in the final months, weeks, and days. Lisa, the woman who died of ‘genug syndrome’, died a peaceful death.
Should medical care attempt to cure an underlying disease until the very last breath? Unfortunately that is the aim and intent of commercial, post-industrial medicine. The decision to change course from prolonging a life to allowing a peaceful death is difficult for all parties involved. We could save healthcare dollars if we limited medical procedures to those that save at least one in every twenty lives. And we could save healthcare dollars if someone of political stature rallied public support for the value of a peaceful death. But life and death are such emotional issues that we rationalize them with great difficulty.
We should all be so fortunate as to live a long, healthy life and die a lucid, peaceful death. But I’ll temporarily close this inexhaustible subject with a thought from Jonathan Dollimore, which I tend to agree with: “… we can begin to understand the vital role of death in Western culture only when we accept death as profoundly, compellingly and irreducibly traumatic.”
Sources and additional links:
(Hover over book titles for more info. Links will open in a separate window or tab.)
The Schopenhauer quotation is the opening of his essay “On Death and its Relation to the Indestructibility of Our Inner Nature” in The World As Will and Representation.
Brian Alexander, “Don’t Die, Stay Pretty. Introducing the ultrahuman makeover,” Wired, Issue 8.01, January 2000
Jennifer M. Soyke, MD, “Genug syndrome,” JAMA, June 11, 2008, 299(22) : 2606.
While writing this entry I found a blog post that has a similar comment on death certificates. Jane Gross, “The Immediate Cause of Death,” The New York Times, October 23, 2008. Jane Gross writes a blog for the Times called The New Old Age, Caring and Coping.
Sharon R. Kaufman, And a Time to Die: How American Hospitals Shape the End of Life
For life expectancy, see Life expectancy at birth, at 65 years of age, and at 75 years of age, by race and sex: United States, selected years 1900-2005 in the CDC document Health, United States, 2007. (PDF)
For a brief history of hospitals, see the chapter “The Hospital” in Roy Porter, Blood and Guts: A Short History of Medicine.
Philippe Aries, The Hour of Our Death
Daniel Callahan, What Kind of Life: The Limits of Medical Progress
Daniel Callahan, The Troubled Dream of Life: In Search of a Peaceful Death
Jonathan Dollimore, Death, Desire and Loss in Western Culture


Sorry, comments are closed for this post.